
Andrew Lund was just 26 when his heart suddenly stopped beating at a family gathering. Paramedics, taking over for a Good Samaritan on the scene, tried restarting it with electric shock (defibrillation). Once, twice – seven times in all.
There was one last hope, a trip to M Health Fairview and a doctor with expertise in resuscitation medicine and a technology that’s a real game-changer for cardiac arrest patients.
Four days later, Andrew came to: “Imagine waking up in a room, not knowing how you got there, but all of your family and friends are there. Cheering.”
“That life that has stopped, has been broken, can now be put back together again because of what our team does,” says Dr. Tolar.
Introducing the world’s first portable version of an Extracorporeal Membrane Oxygenation (ECMO) machine. It takes the place of your heart and lungs, buying precious time for doctors to bring you back to life.
The technology has been around for a while, but the team in the Medical School, with generous funding from the Helmsley Charitable Trust, made it mobile and packaged it to fit in a fleet of cars.
In just four years, the team and its 20-pound hero are changing the odds of surviving cardiac arrest.
“Cardiac arrest is the most time-sensitive emergency in medicine,” says Dr. Yannopoulos. “We have effectively treated about 240 patients and more than 110 patients are alive today – that’s 110 people who would not be alive without this.”
The team, at the U of M, has added three more ECMO-equipped SUVs to its fleet and is training teams of dedicated physicians to operate them.
They’ve also created a non-profit company – the Minnesota Mobile Resuscitation Consortium – and assembled an unprecedented partnership of healthcare systems under it.
That allows the team of two physicians and a paramedic to meet the incoming patient in outlying emergency rooms, putting this lifesaving medicine within reach of 60 percent of the population in Minnesota.
For people living outside the metro area, there are plans and funding for two large trucks equipped with ECMO and other medical devices – making them, in effect, mobile emergency rooms.
There’s a saying that you should never be friends with your patients,” says Dr. Yannopoulos, who calls every one of his just that. “But we strongly believe that that’s the only way to fight for them.”
“Our hope is that we’re never needed. With a couple of shocks, they get pulses. But when this doesn’t happen, we’re there to throw them a life line.”

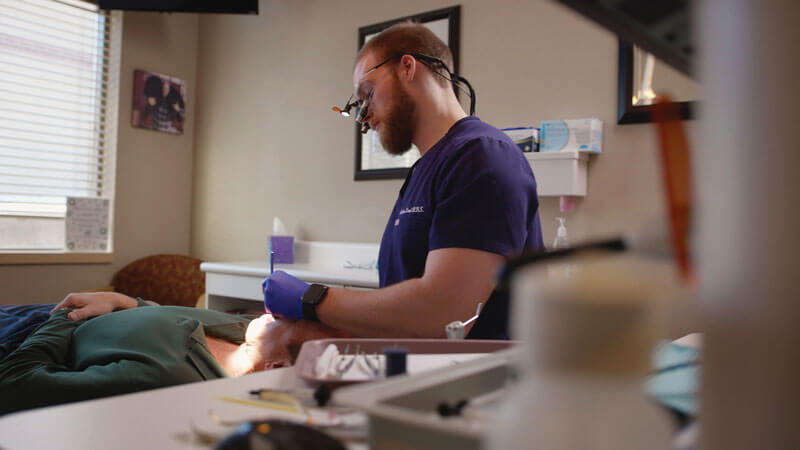
Andrew is fully recovered, working now as a dentist practicing at Duren Family Dental in Burnsville. Doctors discovered – and repaired – the genetic defect that caused his heart to stop. He has an implantable cardioverter defibrillator, as a safety net, but no restrictions. In fact, he was cliff jumping not long after and “nothing happened.”
“I feel like I got a second chance,” Andrew says. “I didn’t realize how good my life was…I’m not afraid of death. But I am afraid of what it would do to my family. This was really tough on them.”
ECMO is also being used to treat patients with COVID-19. M Health Fairview’s first COVID-19 patient – young and otherwise healthy – was put on ECMO as a lifesaving measure. The patient’s lungs were stiff and filled with fluid. Since ventilators work by pushing air with a higher oxygen level with the pressure to inflate the lungs and oxygenate the blood, it was not an option. There was nowhere for the air to go. ECMO was used to oxygenate the blood while bypassing the lungs until they could heal. It worked, and the patient was eventually able to go home. This patient was the first in the U.S. to survive and be able to discontinue ECMO.


Patient
Andrew is a dentist practicing at Duren Family Dental in Burnsville. “Life is very fragile,” Andrew says. “I have a pretty solid faith that I’m here for more of a bigger reason and I look forward to that.”

Dean of the University of Minnesota Medical School
“I started my practice in intensive care medicine 20 years ago. We used to have a machine like this for premature babies but it was as big as a room.”

Medical Director for the Department of Resuscitation at the University of Minnesota
Editing a book on cardiopulmonary resuscitation in medical school, he realized: “That I wanted to try and solve the mystery of sudden death.”
Inspired
University of Minnesota Campus Public Health Office
Center for Resuscitation Medicine
Mobile ECMO
For emergency responders: LifeLink III ECMO Activation Line:
American Heart Association: